PATIENT FOOT & ANKLE QUESTIONS
Join Dr Smith in answering your questions. Post a comment on the Facebook Post “Ask the Surgeon – FOOT and ANKLE” and Dr Smith will read, and answer most questions on here. The current segment is focussing on foot and ankle conditions. Anything from bunions to ankle pain, and everything in between. If you have a question that you have always wanted to ask, now is your chance. Please note that sensitive medical information will not be disclosed on this page. This area will be used for general questions that can be used to help others that may have the same questions as you.
How To Ask a Question
Just click the link above, and you will be brought to the relevant Facebook post. This will be related to the appropriate body part. Ask you question, and you will receive a notification on our Facebook page that your answer has been added to the Ask the Surgeon answers below.
e.g. What is the most common cause for ankle arthritis
Unlike Hip and Knee arthritis, Ankle arthritis is usually due to previous injuries. These may be either recurrent ankle sprains or a previous ankle fracture.
Ankle / Hindfoot Stiffness - Previous motorbike injury and now i have limited movement
In 1974 my ankle dislocated after driving my motorcycle over a wire gate and jammed my foot to the pedal. My skin was not broken but after six weeks the plaster come of and the bones were not in the right place. I had not noticed this for many years but now I have one bone below the ankle on the right foot and none on the left. This has left me with a stiff ankle and having to exercise to walk straight after TKR. After so many years is it worth investigating? There is no pain but limited flexibility.
Thank you for your question. This represents a common scenario. Unlike hip and knee arthritis, the most common cause for ‘ankle’ arthritis is ‘Post – traumatic’ (i.e A previous fracture/break in one of the bones surrounding the ankle, or ligamentous issues).
Certainly from your description of the condition, it sounds like you have developed significant ‘post-traumatic’ arthritis of the ankle joint and potentially the ‘Sub talar’ joint (The joint below the ankle joint). As Arthritis sets in, you will lose your cartilage lining of the joints, and subsequently you lose your ability to move these joints. Arthritis is frequently associated with pain, especially once it reaches the ‘bone on bone’ stage. As the joint surfaces deteriorate, you can also lose the normal ‘architecture’ of your Ankle /Foot, and it may start to take on an unusual shape.
There are many operative and non operative options to consider. I would first of all suggest that you get a weight bearing set of ankle xrays which would help me determine the best course of action.
Pain over Achilles - 3 months following an 'injury'
Hurt my right achilles 3 months ago stepping out of a truck, still have pain in tendon , under heel and in calf muscle even after several visits to doctor and physio. What do you recommend?
Thanks for contacting us. Achilles issues can be a very frustrating injury to have. Issues that may affect the achilles are commonly an achilles rupture (Complete or partial) or achilles tendinosis (Degeneration of the tendon itself). While most cases of complete achilles rupture will be detected at the time of injury, this is not always the case. Certainly more subtle incomplete tears can be easily ‘missed’ during these events.
The Achilles tendon is the main ‘plantar flexor’ of your ankle joint, allowing you to propel yourself forwards during walking and running. Any form of injury to this tendon can result in pain over this area and a feeling of ‘weakness’ when walking.
Achilles tendinosis refers to degeneration of the tendon itself, and can affect either the mid portion of the tendon, or further down towards the heel (Calcaneus) where the tendon intserts. This can be a difficult condition to manage and can have long lasting symptoms similar to what you are describing.
Given that you have experienced a discrete event that started your symptoms, and have ongoing issues, i would suggest that have this looked into further. I would personally arrange an MRI scan to give us the best possible detail surrounding the integrity and quality of the achilles tendon.
Here is some further information surrounding achilles related conditions.
Heel Pain - Causes other than Plantar Fasciitis
With a previous history of hip AVN , should I be concerned about heel pain. GP says Plantar Fasciitis. I do have flat feet so I am thinking PF but at what stage should there be concerns of something else.
Thank you for contacting us. Given your previous uncommon diagnosis of AVN of the hip, i can understand your desire to confirm that your heel pain is indeed plantar fasciitis. The Plantar fascia is a thick broad fibrous band that supports the arch of the foot. It runs from the calcaneus (heel bone) to the toes, and has an important function during weight bearing and ambulation.Plantar fasciitis is a common condition resulting in chronic heel pain. The condition represents irritation / inflammation of the plantar fascia. With progression, tears in the plantar fascia may develop.
The classic presentation of plantar fasciitis is for patients to experience pain under the heel, which is worst when they first get up in the morning, or after long periods of rest.
Common symptoms include:
- Pain at the bottom of the heel
- Pain in the arch of the foot
- Pain that is worse in the morning or after a period of rest
- Gradual progression of symptoms over months
While Plantar fasciitis is the most common cause of heel pain, there are several other causes that need to be excluded. These include a stress fracture of the calcaneus, nerve irritation, achilles tendonitis, and arthritis.
AVN of the calcaneus (Heel bone), while possible, is incredible rare. Certainly common conditions occur commonly, and your description of having flat feet (‘Pes Planus’) increases the likelihood of you having plantar fasciitis.
Here is another Blog article looking at some of the common myths surrounding plantar fasciitis.
Pain at the front of the ankle and 'Giving way'
Right ankle is painful on the left front at the joint just below tibia. I only have partial plantarflexion and the pain often radiates up the inside to the front of the shin. There are times when the ankle gives way completely. Area is tender and swells. Only wear sneakers on flats as ankle gives way with too much of a heal. Thoughts?
Thank you for contacting us. Pain at the front of the ankle (Anterior) can take on several forms. It may be related to a condition called ‘Anterior Ankle Impingment’ . This condition develops when the tibia and the talus (one of the large ankle joint bones) compress against each other during ankle movement. Either a bony spur, or soft tissue scarring may ‘impinge’ in this region resulting in pain.
The ‘Giving way’ that you are describing could be related to a couple of different things. It may be related to the pain that you experience at the front of your ankle, and your body reacts by ‘giving way’. This is often called ‘Pain Inhibition’.
Another possibility is that you have previously injured the lateral ligaments of your ankle joint. These are important stabilising ligaments found on the outer side of your ankle. Injury and deficiency to these structures can result in a loss of balance, and frequent ‘in-rolling’ of the ankle joint. It is common to experience pain in this region also.
If the pain and ‘giving way’ remains problematic, then i would suggest that you have this assessed formally, as there are several treatment options that should be able to help.
Keyhole Bunion Corrections - Recovery
I have a bunion on my Right foot which is giving me grief. Is keyhole surgery available and what is the turnaround time I will be laid up??
Thank you for contacting us. Keyhole Bunion surgery is one of the most common procedures that i perform. I perform this as a day procedure, and you are able to walk on this immediately in a postoperative shoe.
Your recovery time will largely depend on what your occupation is, and what activities you are aiming to get back to. As for most Foot and Ankle cases, i would suggest that you spend the first week trying to keep your leg elevated when you are not walking around.
I would typically see you at the 2 week postoperative mark and remove your dressings. Following this, you are able to transition into roomy supportive sneakers at around the 3 week mark. If you don’t own a pair of these, then remaining in the postoperative shoe is suggested.
If you work in a desk based / sitting role, then you should be aiming to return at around 2 weeks following the procedure. I will see you again at the 6 week mark to get an xray, and your mobility and swelling will continue to improve from there.
Thank you again for your question and we hope the above information has helped!
Post Polio Syndrome - What to expect
Good morning Dr Smith , As a 10 month old child I contracted polio which affects my left leg. I managed pretty good until 1991 when I had an internal rotation of my left leg. Since then I have struggled with my mobility. In 2001 a had a THR to my left leg followed by THR to my right leg in 2002. Due to complications following the THR on my right leg I required multiple surgeries due to repeated dislocations. In January 2018 I had a fall and was taken by ambulance to our local hospital. At the time the doctors diagnosed a dislocation of my left leg. x-rays proved inconclusive and a CT Scan was done. The scan showed that my ankle was not dislocated. However my foot was severly turned in and badly swollen. As a precaution I spent spent 2 weeks in a back slab plaster cast and after a follow up appointment with an orthopedic specialist 8 weeks in a moon boot. On the final orthopedic appointment I was diagnosed with Post Polio Syndrome and told there was nothing more that could be done for me. I now find I am in constant pain with my ankle. Also the strength in my legs has reduced and I’m having trouble keeping my balance when walking. Thank you for your consideration in this rather complex situation that I now face. Any advice would be most welcome.
Thank you for your question relating to post polio syndrome. Polio (‘poliomyelitis’) is an infection caused by the poliovirus. With the introduction of the polio vaccine, this condition has greatly reduced in Australia over the recent decades. While most cases are mild, the virus may also affect the central nervous system leading to paralysis. ‘Post polio Syndrome’ is a condition that affects around 50% of patients that have previously been affected by the poliovirus. In this scenario, over time (usually around middle age), neural cells become inactive over time. This typically results in severe muscle weakness (and wasting) with normal sensation.
Over time, the weakness associated with this condition often leads to contractures or ‘deformity’ of the affected body parts. Having a ‘turned in’ foot is very common in this scenario. There are several different ‘typical’ foot shapes that can occur following post polio syndrome. Initial treatment is often aimed at stretching and orthotic / custom foot wear.
As the deformity increases, surgical options become available. These include release of contractures, tendon transfers, or selective fusions, with the aim of re-creating a more ‘normal’ foot shape to help with foot wear and mobility.
Previous Ankle fracture - Ongoing pain and swelling
In 2008 i fractured my right ankle in 3 places and pulled out of socket had 4 operations on it did something to nerve too but still have problems walking on it and swells up
Thank you for contacting us. The scenario you are describing is very common. It certainly sounds like you had a significant injury to your ankle in 2008. Following this style of injury, it is common to develop pain/swelling years after this original incident.
From your description, it is likely that you have developed a degree of ‘post traumatic arthritis’. This is the most common cause of arthritis around the ankle joint, and can vary in severity. The ‘nerve issue’ that you are describing may be related to the injury itself, or one of the previous operations that you have had. If problematic, this may present as a painful ‘pins and needles’ or a ‘burning sensation’.
Without knowing the exact injury that you sustained, or subsequent procedures, it is difficult to determine your exact diagnosis.
I would suggest that you receive a formal assessment of your current situation and some updated imaging (xrays)
Achilles pain / tendinosis
I have Achilles pain which is worsening.two podiatrists have recommended stretching excercises which has had minimal success. What would be your response?
Thank you for your message. Having chronic pain over the achilles tendon is very common. This is usually related to a condition called achilles tendinosis. This is where the achilles tendon undergoes degeneration and results in regular pain. This may affect the insertion site of the achilles (‘Insertional tendinopathy’) or along the mid point of the tendon itself (‘Non insertional achilles tendinopathy’). Typically soft tissue based imaging modalities (Ultrasound or MRI) will show these features for these select cases.
A feeling of ‘tightness’ of the calf muscles is usually present, and patients often notice a ‘bump’ or enlargement of the tendon. Difficulty with shoes rubbing is common.
Achilles tendinosis is best managed with an active management plan.
An initial period of ‘rest’, anti-inflammatories, and achilles stretching, is followed by a structured strengthening program.
If the symptoms fail to settle, surgical debridement of the degenerative tendon and removal of any excess bony protuberance or bursitis (inflamed tissue) may be performed.
Pain under the arch of the foot
I get a sharp pain just under the left arch of my foot and just above it when i walk on the treadmill, i stopped using the incline on the treadmill, the pain is very intense at times…. and sometimes in the morning my foot is still very sore …. it doesn’t happen all the time …
Thank you for contacting us. It sounds like you are experiencing pain over your ‘plantar fascia’. The Plantar fascia is a thick broad fibrous band that supports the arch of the foot. It runs from the calcaneus (heel bone) to the toes, and has an important function during weight bearing and ambulation.
The classic presentation of plantar fasciitis is for patients to experience pain under the heel, which is worst when they first get up in the morning, or after long periods of rest.
Pain in the arch of the foot
Pain that is worse in the morning or after a period of rest
Gradual Progression of symptoms over months
Conservative options to manage plantar fasciitis include stretching exercises, shock wave therapy, and consideration of an injection. We also offer selective keyhole releases of the thickened fascia if the above measures have not been beneficial
Rheumatoid Arthritis and Peripheral neuropathy
Hi im 65.have diebetes. Rheumatoid arthritis..and peripheral neuropathy. Nerve damage..my feet and ankles are in pain every day..i get up out of bed or a chair and its like walking on bone..gets a little better after movement.but stays painful.. methotrexate for rheumatoid .metformin for Diabetes.
Thank you for contacting us. You have an unfortunate combination of conditions that will predispose you to issues in your foot and ankle. Rheumatoid arthritis is a chronic inflammatory disorder that frequently affects the joints surrounding the ankle and foot. Over time, the ‘arthritis’ often results in deformities of the affected joints and inflammation of the joint lining.
Diabetes is a common cause of peripheral neuropathy affecting the feet. This can present in several different fashions, including a loss of sensation, a painful ‘burning’ sensation, or a change in shape of the foot related to an imbalance in the muscles surrounding the foot.
I would suggest that you start by getting a weight bearing foot/ankle xray to look at the severity of any underlying arthritis. In general, treatment is aimed at optimising your medical management of your rheumatoid arthritis and diabetes, and consideration of the specific management of the joints affected. Both conservative and surgical options are available depending upon your specific presentation.
'Ball of foot pain' | Metatarsalgia
Good morning Dr. Smith, I have terrible corns on the pads just below my toes, I wear orthotics and have a podiatrist shave them, but they’re back within a couple of weeks,is there anything else I can do,as it’s on both feet and very painful to walk.thank you.
Hi. Thank you for contacting us. It sounds as though you have a condition called ‘metatarsalgia’ which means ‘ball of foot pain’. The fact that you are describing significant callus formation within the ball of your foot, may indicate that you have a biomechanical cause for this. If you have a relative lengthening of your 2nd, 3rd, or 4th metatarsal (foot bones) in comparison to your 1st metatarsal (Great toe), then increased pressure will be placed through this region of your foot. Having a big toe that fails to take the appropriate force during walking (either due to a bunion or arthritis of the great toe), will also transfer the forces through to the ball of your foot. This may be the reason that your ‘corns’ continue to return despite having the regular shavings.
I would recommend that you start with some weight bearing foot xrays. If the conservative measures are failing to improve your symptoms, there are keyhole techniques available to help take the pressure of the ball of your foot.
Post traumatic Ankle pain
I have broken my left ankle twice and torn all my ligaments and tendons at a later time trying not to re brake the ankle. The latter was in January of 2016 and it has still not healed properly. I have flat feet, am pigeon towed and suffer from peripheral neuropathy. Is there anything that can be dun to improve my situation? I can’t walk as far as I use to and find shoes unbearable especially when worn for more than a few hours, laces are the worst. I also get a lot of pain in the ankle and loss of mobility in the joint. Thank you in advance.
Thank you for your message. Your description sounds similar to one of the other recent questions that we received in relation to ongoing pain following a previous injury. This is most likely ‘post traumatic arthritis’, which is the most common cause of arthritis affecting the ankle. For more information regarding this, please see my response above.
Specifically in relation to your difficulty with shoe laces, this may be related to bony ‘osteophytes’ across the top of your foot. These are bone spur formations that are often seen in the setting of arthritis. They can result in a chance of foot shape, and difficulty wearing normal footwear. They can also result in compression of some of the skin nerves that run along the top of your foot.
I would start with a set of weight bearing foot and ankle xrays to help guide the specific diagnosis.
Ankle pain and Instability
For many years now I have had issues with my r ankle (when younger also had Achilles Tendonitis in this ankle) ankle was quite unstable to the point of almost rolling it every couple of days when walking on unstable ground…went to physio for 6 months which helped stabilise the ankle, however I now find that if I do too much walking etc I get pain under the ankle bone (side of foot). Any suggestions on next step would be appreciated.
Hi and thank you for your message. Your original description of frequently ‘rolling’ your ankle is often due to an insufficiency / rupture of your ‘lateral ankle ligaments’. These are the main stabilising ligaments of the ankle. One of the consequences of having multiple injuries to these structures is that it can result in the development of inflammation and scarring within the outer /lateral gutter of the ankle joint. This can result in a condition called ‘impingement’.
If you have had damage to the cartilage lining of the ankle joint, you may also have developed arthritis. Multiple ligament injuries is one of the leading causes of ankle arthritis.
I would suggest that if you are having ongoing issues with pain, that you arrange a weight bearing xray to start with. This will provide information relating to any development of arthritis or ‘bony’ impingement. You may also benefit from a MRI to assess for any soft tissue ‘impingement’ on the outside of the ankle.
I would suggest that you then arrange a referral to a specialist for a formal assessment and management plan. Hope this information helps!
Rheumatoid Arthritis and Foot/Ankle Pain
Hi im 60 and have Rheumatoid arthritis my right foot is so painful at the top of my and around the ankle some days the pain is so strong it goes from my big toe fight across the top to my ankle dont wear shoes with heels always wear airfflex
Hi and thank you for reaching out to us. I have covered this issue in one of the previous questions. Rheumatoid arthritis is a chronic inflammatory condition that frequently affects the small joints of the foot and ankle. It can result in debilitating pain and a change in shape of the foot structure.
Your description of pain across the top of the foot/ankle may indicate that the Rheumatoid arthritis is affecting the larger joints surrounding the ankle as well as possibly the 1st MTP joint (large joint of the big toe).
The management of this condition is a combination of medical and possible surgical management. Medically, i would ensure that you have optimised your medical management of this. I would then arrange a weight bearing xray of your foot and ankle to determine the current joints that are affected and to what severity.
There are many surgical options available to help alleviate your pain, and I would be more than happy to review these with you
Recurrent dislocations of little toe
Hi I’m 54 and I have problem with dislocation of my little toe ( left foot only ) 6 times already . It’s dislocating very easily, would fusion fix my problem? Thank you
Thank you for reaching out to us. Your situation certainly sounds like a frustrating process. Dislocating your toe 6 times indicates that you have likely ruptured some of the important stabilising ligaments of the. affected joint. The ‘toe’ is made up of three phalanges (bones) and a longer metatarsal bone. This creates a Metatarsophalangeal (MTP) joint, and a proximal and distal interphalangeal joints (PIP and DIP joints)
The first part of my assessment would be determining which joint is involved and having issues with stability. The PIP and DIP joints can easily be ‘fused’ to prevent any further dislocations. The MTP joint would require a different strategy to provide stability, which may involve a ligament reconstruction.
Given that this has happened 6 times, i would suggest that you be seen and assessed. I would start with a weight bearing xray, but you may also require an MRI scan to assess for soft tissue (ligament) injuries around the joints.
Calcium deposition achilles and plantar fasciitis
Hi Dr Smith
I have tightening of my Achilles, calcium and plantar fasciitis. What is the best treatment?
I have tried physio with shock therapy and I get relief for a week to two weeks then it’s back.
Thank you
Hi and thank you for your message. It sounds as though you have a couple of coexisting conditions. The tightness in your achilles with ? calcium deposition, may possibly be affecting the insertion point of your achilles tendon, in a condition termed ‘insertional achilles tendinosis‘. This usually results in pain over the achilles insertion into the heel bone (calcaneus) and a general feeling of tightness in the tendon. There may also be a bone spur present in this location with calcium deposition.
Plantar Fasciitis is a very common condition resulting from degeneration of the origin of the plantar fascia. Small tears may also develop in this region.
Shock wave therapy has been described for both conditions as a treatment option. Unfortunately, it is not always successful. I would suggest that you be seen for a formal assessment to help determine the predominate pain generator in your foot. Subsequent imaging may be warranted (such as a MRI scan).
If you have exhausted this nonoperative options (physio, shockwave therapy), there are minimally invasive surgical options available.
Recent Ankle Fracture - Risk of developing arthritis
I broke my leg in March and now have pins etc in lower leg above ankle. I have had ankle.reco structuon prior to this leg break and it would swell up quite alot..I am just concerned that in years to come I will have complications…Will this be the.case
.thankyou.
Thank your for contacting us and providing an xray. Your xray indicates that you sustained a significant injury that involved the tibia (shin bone) as well as the ankle joint. When ever the ankle joint is involved with a fracture (‘break’) you are at risk of developing arthritis down the track. In fact, the most common cause of ankle arthritis is following an injury such as yours.
In the short term, i would encourage you to continue with your rehabilitation and start to regain your range of motion and strength, that are lost following such an injury. The speed at which you develop arthritis (if at all), is difficult to know. Not all patients with arthritis are symptomatic, and i would plan to manage you based on your symptoms, if and when they develop.
Painful Bunions
My feet r always sore. I have bunions. Doesn’t matter what shoes I wear, I have no comfort. My ankles hurt when I walk for a period of time. I was a waitress for 25 years so on my feet quite a lot. Can u help?.
Hi, and thank you for contacting me. Bunions are a very common condition that frequently results in pain. Please read this article that i have previously written regarding the different ways in which your bunions can affect you.
There are several potential sources of pain:
Prominent Medical Eminence
A painful red callus may form directly over the inner aspect of the bunion. This is typically the result of the bunion rubbing against the inner side of the shoe.
Transfer Metatarsalgia
Progressive bunion deformity can result in reduced ‘function’ of the great toe. This may transfer the weight bearing forces to the undersurface of the 2nd and 3rd metatarsal heads (lesser toes) resulting in ball of foot pain.
Degenerative Hallux Valgus (Bunion)
Over time, some patients suffering from bunions will develop arthritis of their great toe (1st MTP joint). Resulting pain and stiffness typically occur.
Personally, i perform my bunion corrections through a ‘keyhole’ technique that is designed to alleviate the pain that you are experiencing, whilst providing a cosmetic solution through tiny incisions. Both feet may be addressed at the same time, and you are able to weight bear immediately.
If you would like to have a formal assessment, please contact my rooms (7099 0188) at your convenience.
Heel pain worse when getting up from sitting
I have extremely sore feet, especially when getting up after being seated for a while, I really struggle to walk and the pain is quite intense, after I get moving it seems to ease. Mainly both heels, but also on top of my foot running back from my little toe
Hi, and thank you for your message. Your description of the pain being worse after you have been seated, and it affecting your heels, sounds characteristic for plantar fasciitis. I have covered this condition in some of my recent responses. For further details, please click here
Thank you for getting in touch with us.
Ongoing pain following an ankle sprain 9 months ago
Hi there I sprained my ankle back in September I’ve have a cortisone injection but still no better. When they did the ultrasound they said there was a lot of fluid. It is constantly swollen and aching. What do you think could be the problem
Hi and thank you for contacting us. Most ‘Simple’ ankle sprains will settle down in short space of time (4-6 weeks). Unfortunately, you have been experiencing pain for 9 months following this injury. I classify these injuries as ‘complex’ based on this description alone.
There are many causes for ongoing pain following an ankle injury. Please see this link for further information. Bony, soft tissue, and ligament causes could be contributing to your ongoing pain. Potential bony issues include missed occult bony fractures, cartilage injuries to the ankle joint, and loose bodies within the joint. Soft tissue issues include ‘impingement’ due to scarring within the ankle joint, as well as inflammation of the joint lining. Tendon issues may be related to the tendons that run along the outside of the ankle (peroneal tendons), or a high ankle sprain (syndesmosis injury).
I would certainly be suggesting that you have your ankle formally assessed by a specialist, and you will likely require up to date imaging (xray +/- MRI scan).
Once we have a diagnosis, we can start to formulate a management plan for you.
Previous severe trauma with nerve damage and a change in foot/toe shape
Hi there,
Almost 26 years ago I almost cut my leg off just above the knee from behind, cutting everything except the skin at the front, and front 1/2 of the bone,
As a result, I’ve got limited use of that leg,
But I suffer more so from drop foot,
My up / down & side to side movement of my foot is only a clickly moment from 11 – 4 o’clock,
My ankle is often very swollen, I have claw toes,
As nerve ends are everywhere, I struggle with sensations on the foot….
any help here.?
I use to wear a brace for the first few years after the accident but it left my foot very sore and bruised, so I stopped wearing it,
Hi and thank you for contacting us. It certainly sounds like you had a very significant injury many years ago. As a consequence of this, you have most likely severed several of the key nerves that supply the muscles/tendons controlling the ankle and foot. You have likely also injured the tendon/muscle units themselves.
One of the consequences of long term nerve injury, is that you develop an imbalance in the muscle forces acting across these joints. This may result in the ‘clawing’ of the toes that you have described. The Ankle and hind foot may also change in shape secondary to this nerve injury. Your ‘Foot Drop’ may be due to a combination of muscle/tendon injury as well as a lack of appropriate nerve supply.
This represents a complex scenario to manage. We certainly have surgical options available with the aim of providing you with a stable foot that you are able to walk on. If you have lost the sensation in your foot, it is unlikely that you will recover this. If this loss of sensation (‘paresthesia’) is not painful, then I would not recommend you start any particular medications. If you are experiencing a ‘neuropathic pain’, such as burning, nerve irritation, then there are specific medications that may help you.
Given the complexity of your case, I would suggest that you arrange an appointment with a specialist for a formal assessment. As always, I would be more than happy to see you, if you would like to schedule an appointment.
Missed fracture - ? Development of a malunion (Abnormal angulation of the bone)
I broke my left ankle in my late teens playing softball. Unfortunately the break wasn’t discovered until a few years later as the initial diagnosis was a sprain. A specialist thought about breaking it + trying again but was only 50/50 outcome so decided against it. I’m on my feet all day in my current job + when I go home after 9/10 hours at work it swells like a softball + throbs during the night while trying to sleep. Any suggestions would be grateful
Hi and thank you for the message. Given that your original diagnosis was delayed, and you were being considered for a ‘re breaking’ or ‘osteotomy’, it is likely that your original fracture healed (united) in a different position. This is termed a malunion. In your younger teenage years, fractures around the ankle may affect the growth plate. This can result in ‘growth arrest’ of part of your growth plate, resulting in an abnormal angulation to your ankle as you continue to grow. If this injury occurred in your late teenage years, then it is unlikely that your growth plate was affected, as you would have stopped growing already.
I am unsure of your current age, however if you have lived with a ‘malunion’ for many years, this will result in abnormally high stresses being placed across your ankle joint in certain areas. One of the consequences of this, is the development of arthritis.
I would start by arranging a weight bearing xray of your foot and ankle. This will provide us the information that we need to help make a diagnosis. I would then suggest that you get a formal assessment and we can tailor a management plan from there. Hope this helps. THanks
Ankle 'Weakness' - No longer able to play sport
Both of my ankles are very weak.. I can’t play any sport because of it. I can be walking normally and they will just give away on me and I am on the ground in pain and can’t do a thing.. with many trips to the doctors and to be told nothing can’t be done I have got this for life is not what I wanted to be told
Hi and thank you for your message. One of the main reasons for having ‘ankle instability’ is having previously injured your lateral ankle ligaments. These are the main stabilising ligaments on the outside of the ankle. If you have had multiple ankle ‘inversion’ injuries in the past, your ligaments in this area may be chronically ruptured / deficient. These ligaments are important providing stability when you are walking on uneven ground, or changing direction quickly during sport. Click here for more information regarding this.
Having weakness of the muscles / tendons that surround the ankle joint, can also result in the feeling of your ankle ‘giving way’. Attempts at strengthening these structures may help with the ‘giving way’ that you are describing.
Ultimately, i would need to take a further history and examine your ankle to pin point the likely cause of your weakness, and help formulate a management plan for you.
Thanks again for contacting us!
High Arch Feet - Orthotics
Hi. I have extremely high arches which makes my hips hurt. I used to wear orthotics but haven’t had more made since i was at school. I cant really afford them. What will happen long term if i just do nothing?
Hi and thank you for contacting us. Having very high arches is called ‘Pes Cavus’. Some people naturally have very high arches and it causes them little issues. Other patients have associated foot pain. This may be related to pressure overload through the forefoot (metatarsalgia), plantar fasciitis, or issues relating to the hindfoot such as achilles pain and arthritis.
On other occasions there are known causes for developing pes cavus. The cause and deforming mechanism underlying pes cavus is not completely understood. Muscle weakness and imbalance in neuromuscular diseases, residual effects of congenital clubfoot, post-traumatic bone malformation, contracture of the plantar fascia, and shortening of the Achilles tendon, have all been described as potential causes.
While orthotics are often prescribed an provide good pain relief, if you have minimal symptoms without them, then i would not be suggesting that they are a ‘must have’.
If you develop significant pain within your feet, then i would be suggesting that you seek a formal review/opinion. Orthotic use may be an important component of this treatment.
Achilles pain -Home based exercises
How long does Achilles pain last and what can I do at home to relieve
Hi and thank you for contacting us. The achilles pain that you are referring to may be related to achilles tendinosis. This is a condition where the tendon undergoes degeneration resulting in pain within this region. It is often also referred to as achilles tendinitis. The condition has a varied course, with some people experiencing relief within weeks, and others have a protracted course lasting years.
During the early phase, we often suggest that you try to reduce the pain with basic modalities such as rest (avoid aggravating activities), ice, compression, and elevation. A small heel wedge in your shoe can help take the tension of your tendon during this period.
After you have recovered from this acute phase, treatment is aimed at stretching and ‘loading’ the achilles tendon. ‘Eccentric’ achilles exercises are often prescribed with good benefit. ‘Eccentric’ muscle action is where the muscle fibres lengthen (rather than shorten) during contraction. For the achilles, this is usually done with a controlled heel dip. To do this, stand on a step with your toes, and carefully drop your heel below your toe height while contracting your achilles. Repeat these.

Following this a specific strengthening program can be commenced. As always, if possible, having this program supervised by a physiotherapist, sports physician will be beneficial.
Tailor's Bunions - 'Bunionettes'
I have Tailor;s bunions in both feet. How successful would surgery be and how long would recovery be?
Hi and thank you for contacting us. A Tailor’s bunion is a colloquial term used to describe a ‘bunionette’ deformity. This is where someone has a ‘bunion’ of the little (5th) toe. There are several different types of bunionette deformities based on your xray appearance. These include an enlarged 5th metatarsal head, an abnormal bow to the 5th metatarsal (bone), or an abnormally wide angle between the 4th and 5th toes.
My preference is to perform bunionette corrections using a keyhole technique. If you have an enlarged metatarsal head, a simple ‘shaving’ of the prominence, may be all that is required. If the xray displays a bowing of the bone, then a corrective osteotomy (realigning) of the bone may be required. This can usually be done via a keyhole technique. This is done as a day procedure and you are able to weight bear on this immediately in a postoperative shoe. The success rates following this are high.
Thank you for submitting you question and we hope the above information is helpful
Hammer toe in a 27 year old
Hi im 27 yrs old, and have hammer toe, what is the best way to fix relieve the toes? I also walk with my fert outwards and have trouble straightening them any ideas
Hi and thank you for contacting us. Hammer toes are a common condition that can affect any age group. They commonly affect the 2nd toe, but multiple toes may be involved. They can be found in isolation, or secondary to a bunion deformity of the big toe.
One of the biggest issues that patients with Hammer toes find, is that they have difficulty with footwear, with rubbing occurring over the top of joint. Pain under the ball of the foot (metatarsalgia) may also be present. Aside from arranging to wear ‘roomier’ shoes, Hammer toes are often managed with a procedure to realign to the toe. This is performed as a day procedure and is minimally invasive. You are able to walk following the procedure.
Walking with your feet turned out is termed ‘External foot progression angle’. This may be a normal varient and is often related to the rotational alignment of your hips / tibias. You would require a formal examination to determine the location of your ‘rotation’.
I hope you find this information useful!
Heel Spur - How to remove
What’s the easiest way to get rid of a heal spur please?
Hi and thank you for your message. There are two types of common heel spurs. While both arise from the calcaneus (heel bone), they are found in different locations with different consequences.
The first is the ‘Plantar calcaneal heel spur’ as seen in the image below.
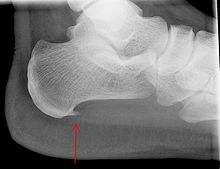
I have recently written a blog article on this topic, so please click here to read this. The crux of a spur in this location, is that while many patients have a heel spur in this area, many are not symptomatic. There is however an association with plantar fasciitis and heel pain.
The second common form of heel spur relates to the insertion of the achilles tendon in a condition termed ‘insertional achilles tendinopathy‘. This spur is found at the back of the calcaneus, where the achilles tendon attaches.
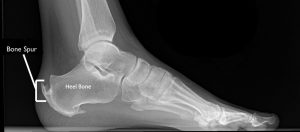
It is often associated with pain in this region, and a tight achilles. If conservative measures fail to improve your symptoms, then a debridement and removal of spur is frequently performed. This is done as a day procedure.
Thanks again for your question!
Foot Drop - Wearing an Orthotic
I have permanent foot drop caused by compartment syndrome caused by hyper leg extension/compartment syndrome. I wear a ankle/foot orthotic by day. Should I be wearing it at night also?
Hi, and thank you for contacting us. A ‘Foot drop’ is the inability for one to be able to keep there foot ‘up’. This is typically related to a dysfunction in a particular muscle called the tibialis anterior muscle, which is responsible for this action. The cause of dysfunction may be permanent loss of the muscle fibres / tendon, or from a neurological cause (injury or condition).
It sounds as though you have been prescribed a device that is aimed at keeping your foot ‘up’ while you walk. The aim is to prevent you for tripping over, and to help with your mobility. One of the most important steps in managing a footdrop is to ensure that your ankle joint remains ‘supple’. I.e despite you not being able to ‘actively’ lift your foot up on its own accord, you may be able to achieve this with the use of your hands. The aim of the AFO is to prevent you developing an equinus contracture also. There are specifically designed low profile braces that can be worn at night to hold your foot in the appropriate position during these hours. While you will not develop a severe contracture overnight, the more compliant you are with wearing your brace, and exercises, the less likely you are to develop a contracture.
I also perform surgical procedures for patients with permanent foot drop if they are an appropriate candidate. Tendon transfers may be possible, where a tendon is transferred to the top of your foot, to give you some ‘active’ control in preventing your foot from dropping down. You would require a formal assessment for this.
Thanks again for your question
Arthritis and collapse of the foot arch
I have osteoarthritis and a collapsed arch on my left foot…pain is excrutiating. Is there anything besides orthotics to help?
Hi and than you for contacting us. From your brief description, it sounds as though you may have a condition called ‘midfoot arthritis’. This can result in the development of painful arthritis across this region with subsequent collapse of your foot architecture.
Given that you are in extreme pain, despite orthotics, i would be suggesting that you obtain ‘weight bearing xrays’ of your foot and ankle, and seeking out a formal assessment. We have surgical solutions (Such as a realignment procedure or fusion of selective joints) for this condition that is aimed at relieving your pain.
Kind Regards
Tailor's Bunion - Painful Feet
Can you tell me about tailors bunions? I believe I have them – swelling / growth beside little toes and lots of pain after working on feet.
Hi, and thank you for contacting us. Tailor’s bunions are a prominence / ‘bunion’ affecting the little/5th toe. While there are several different types, the main issue that these cause are a painful prominence on the outside of the foot, that causes discomfort and difficulty wearing shoes.
In a similar fashion to ‘regular’ bunions, i correct these using a keyhole technique as a day procedure. I would suggest that we start with a weight bearing xray to determine which ‘Bunionette’ pattern you fall into.
As always, i would be more than happy to review you.
Ongoing pain and restriction in movement following an ankle injury
My husband broke his right ankle, he has had issues with rolling his ankle and it being very painful when it happens. The rolling of the ankle all happened before he eventually broke the same ankle. When he broke it, it swelled up ALOT and he was in hospital for 4 days due to them being able to get a clear Xray, so they eventually did an MRI. So, this happened back in the middle of March this year, he still has some mild swelling, restriction of movement and some pain. I have said he needs to go to a physio to start getting some strength back into it. But he “is too busy”. He had it in a moon boot for around 8 weeks, as he is self employed and needed to be mobile…… what do recommend going forward to help him heal better (as he won’t stay off his feet) and gain more strength back into it. Thankyou
Hi, and thank you for contacting me. It sounds as though your husband was experiencing recurrent ankle sprains in the lead up to his fracture. It doesn’t sound as though he required surgery at the time of his ankle fracture, so this may have been either an un-displaced fracture or an avulsion injury (where the ligament pulls a small section of bone off).
Certainly, undergoing a period of rehabilitation with the physiotherapy team is often the most appropriate step for patients recovery from an ankle injury. The ongoing ‘swelling’ and restriction in movement is not uncommon. I would suggest that he try to find time to visit a local physiotherapist to help put together a strengthening program for him. If he is still having issues with pain , swelling, or ongoing ‘rolling’ of the ankle, then i would advise that he have this formally assessed. For patients that continue to sprain their ankles, they may require a lateral ligament reconstruction which is designed to stabilise this portion of the ankle joint and prevent further injury.
Thanks again for contacting us.
Leg length discrepancy following a hip replacement
After a hip replacement the operated leg is now one 1 cm shorter than the other one. Is it possible to build up the shoe to match the other leg?
Hi and thank you for your message. It is not uncommon for patients to have a slight ‘leg length discrepancy’ following hip replacement surgery. Typically, when the legs are within 10mm of each other, the patient will not be able to appreciate this difference. In fact, when measured, many people have a natural difference between the two legs.
If you have noticed that you are ‘shorter’ on your operative side, then it is certainly possible, and suggested, that you consider a ‘shoe raise’ on that side. Before getting this ordered, i would suggest that you have an assessment for the exact functional ‘leg length discrepancy’ that you have, so that the orthotist can accurately build up your shoe to balance you out.
Kind Regards
Nerve Pain following a Lisfranc injury
Is there anything that can be done to help with nerve pain following surgery for a Lisfranc Injury ? 2.5 yrs later I still suffer from daily pain.
Hi, and thank you for contacting us. A Lisfranc injury is a significant injury that occurs to your midfoot. The named ligament (Lisfranc ligament) runs between two bones on the inner (medial) side of your midfoot (Medial cuneiform and base of 2nd metatarsal).
There are several different techniques that can be used to ‘stabilise’ this region following this style of injury. If metal work (screws/plates) are used, then these will often be removed around 4-6 months following the original surgery.
One of the superficial nerves (Deep peroneal nerve) runs over this region of the foot and supplies skin between the big and 2nd toes. This can be injured / bruised as part of the original injury or surgery in the area.
There are several reasons for pain in this region, and i would first want to exclude that you havnt developed arthritis in this region, or an ‘osteophyte’ (bone spur) that is impinging on the nerve. This would require up to date imaging of the foot. If the pain is neuropathic (nerve related) with no obvious surgical solution, then there are some medications that can be used to help target this style of pain. Lyrica is good option for this.
I hope the above information is useful, and as always, we would be happy to review you if you would like.
Kind Regards
Lupus (SLE) and Heel pain
I have sore heals i also have lupus
Heel pain may occur in patients with an underlying systemic inflammatory disorder, such as lupus or rheumatoid arthritis. The inflammation that occurs during Lupus, can affect the plantar fascia, which is a thick band of connective tissue running along the sole of the foot. Over time, the plantar fascia can undergo degeneration and micro tearing, resulting in pain felt underneath the heel.
Typically the pain is worse in the mornings, and when taking your first few steps of the day. Please click here for further information regarding plantar fasciitis.
Thank you again for your question and we hope the above information is helpful!
Painful achilles - 'Non insertional achilles tendinosis'
Hi, i have had a swollen bulge on my achilles for almost 2 years. Have tried physio & been to a specialist who has just said isometric exercises. Doing this has caused severe calf issue in other leg. Would appreciate any advice to help both! Going overseas shortly & need to be well!
Hi, and than you for your message. From your description, it appears as though you have ‘non insertional achilles tendinosis’. Patients tend to describe having pain over the achilles tendon, swelling (and possibly a ‘bulge’ like you are describing), with associated stiffness. The majority of these cases can be managed with conservative care successfully. Unfortunately, some patients fail to improve, and may require a small surgical procedure.
In the first instance i would ensure that you have removed any precipitating factors (such as a particular exercise that you do that may make it worse). Physiotherapy is aimed to address the muscle weakness and ‘stiffness’ that can develop. Eccentric exercises are often prescribed. Please see the below image for an example of this with ‘heel drops
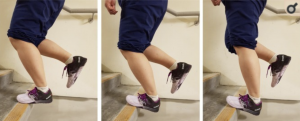
Other conservative treatment options include shock wave therapy and a ‘High volume injection’ for paratenon (the lining of the achilles tendon) stripping.
Given that your symptoms have been present for 2 years. i would suggest you have a formal assessment for your condition. I hope the above information is helpful.
Please click here for more information.
Pain 8 years following a lateral ligament Reconstruction
I had lat lig recon in my left ankle 8 years ago. I have had no trauma to it since. However the pain has returned. I have stability in my ankle, but I am starting to put more weight on my other foot. Throbbing pain from my ankle up to my knee then to my hip. All on the left side.
Hi and thank you for contacting us. Your lateral ligament reconstruction would have originally been aimed at restoring stability to the outside of your ankle joint to prevent you from ‘rolling’ your ankle. Given that you have not had any further issues with the stability of this ankle, then this sounds like it has been successful.
The issue that you are currently facing, is that you have pain which has returned. There are several possibilities for why you have developed pain within the ankle again. Certainly one of the most likely issues, is that you may have developed a degree of arthritis within the joint itself. One of the leading causes of ankle arthritis is having had previous trauma to the region. This can either be in the form of recurrent ankle sprains, or a fracture. In the early stages of arthritis, you may develop bone spurring (osteophytes) at the front of your ankle. This can lead to a condition called ‘Anterior Impingement’. Associated joint lining inflammation (Synovitis) may develop leading to pain.
I would suggest that you arrange a formal assessment and i would be ordering some weight bearing xrays of your ankle. This will help provide us the information that we need to confirm a diagnosis and develop a management plan for you.
I hope the above information helps!
Toe Arthritis options
Can arthritis on a toe be fixed or the joint replaced?
Hi and thank you for your comment. While i would need to gain further information regarding which joint was involved, to give a more precise opinion, i am able to make some generalisations for you.
The big toe (Hallux) has two main joints that can be affected by arthritis. The most distal one (closest to the toe tip) is called the IP joint. The joint closer to the middle of the foot, is called the MTP joint and is frequently affected by arthritis. There are several grades of arthritis that may affect the MTP joint. In the early stages, only part of the joint is involved, the movement of the joint is largely preserved, and you may have developed a bony spur (osteophyte) in the area. Techniques to help this stage include removal of the spur and a debridement of the joint. As the arthritis progresses, and the joint loses it’s movement, two options remain. The first is an arthrodesis (fusion) of the MTP joint to help alleviate your pain. The second, is a synthetic ‘hemi arthroplasty’ where a ‘spacer’ is inserted to alleviate the ‘bone on bone’ nature of the arthritis, whilst maintaining movement.
Arthritis in the smaller toes may also be addressed depending on the location. The smaller toes have 3 joints. The DIP and PIP joints are able to be fused (‘fixed’) to help alleviate the pain. The more proximal joints (MTP joints) require alternative options, as fusion of these joints is not indicated.
Thanks again for your question, and we hope you find the above information helpful.
Kind Regards
Ganglion adjacent to the ankle and 'Ball of foot' pain
I have a ganglion by my ankle that I have had for couple of years ! Gives me really sore ankle and by end of day is quite swollen!
Also with the other foot I get pain under the toes/ball of foot that I have had a cortisone injection in a couple of times!
Is both of these problems treatable ?
Hi, and thank you for your recent question. I will start by addressing your ganglion. A ganglion is a benign soft tissue lump (often hard) that can arise from an adjacent joint or tendon sheath. It represents an ‘out pouching’ of fluid that can get trapped, resulting in the palpable lump. Some people notice that the swelling can increase and decrease in size over time. The ganglion can cause pain in itselfm, particularly if it is compressing on adjacent structures. Sometime the underlying joint or tendon may also have undergone a degree of degeneration (arthritis / tendinosis) that can contribute to your pain. When these ganglion are causing symptoms (pain etc), they can be removed via a day procedure.
‘Ball of foot pain’ is called metatarsalgia. There are many causes for this condition that range from an abnormal biomechanical issue with your forefoot, through to localised conditions affecting the lesser MTP joints or adjacent nerves (ie neuromas). Each of these specific conditions have a certain management plan available. The most important step, is to acquire a formal assessment so that one can pinpoint the cause of your symptoms and develop a management plan. While corticosteroid injections can certainly be beneficial in some circumstances, i would avoid repeated injections without a clinical diagnosis. For more information on ‘metatarsalgia’, please click this link
Kind Regards
Bunion and adjacent hammer toe
Hi and thank you for your message. A combination of a bunion deformity and adjacent hammer toe is a very common situation that i treat regularly. I perform all of my bunion corrections utilising a minimally invasive ‘keyhole’ technique. In a similar fashion to bunions, hammer toe deformities can range from mild, moderate, to severe. Depending on the severity of the hammer toe, various surgical options are available to correct the adjacent hammer toe deformity. The aim of the correction is provide pain relief, and help ‘straighten’ the toe out to prevent it from rubbing on your shoes.
Combining the correction of the bunion, with the hammer toe, does not alter the postoperative course, and patients are still able to weight bear immediately in a postoperative darco shoe.
If you would like to have a formal assessment, please contact Kim (my PA) on 7099 0188.
I hope this helped answer your question.
Kind Regards
Mike
Disclaimer: Please note that this is general advice only - for more information, please consult your regular doctor, or obtain a referral to see a specialist orthopaedic surgeon.
Orthopaedics 360
Orthopaedics 360
P: (08) 7099 0188
F: (08) 7099 0171
Southern Specialist Centre
Orthopaedics 360
P: (08) 7099 0188
F: (08) 7099 0171
Health @ Hindmarsh
Orthopaedics 360
P: (08) 7099 0188
F: (08) 7099 0171
