Orthopaedics 360
An achilles tendon rupture is most frequently seen in middle aged recreational sporting enthusiasts. It can occur spontaneously, but can also be seen in people that have had a vague pain or ‘tightness’ at the back of their calf for a period of time.
Achilles tendinitis / tendonitis actually refers to inflammation of the achilles tendon. This is a commonly used term amongst the general public, however we now know that the source of pain in this condition, is secondary to tendon degeneration, rather than ‘inflammation’. This is called Achilles Tendinosis.
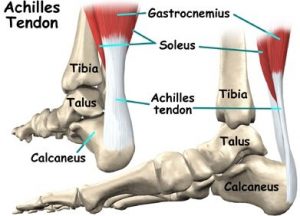
Anatomy of the Achilles
The achilles tendon is the thickest tendon in the body. It is the tendon at the back of the leg that connects the calf muscles (Gastrocnemius and Soleus) to the Heel bone (Calcaneus) which allows your foot to ‘plantarflex’. Propulsion during running and jumping require an intact achilles tendon.
How to Diagnose an Achilles tendon Rupture
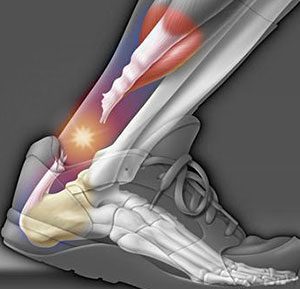
Patients who experience an achilles rupture typically describe hearing a loud ‘snap’ with immediate pain at the back of the ankle, and falling to the ground. Often people describe the feeling of being ‘kicked’ in the back of the ankle, but when they look around, there is no one near them.
A physical examination will reveal a palpable defect in the tendon, at the site of the tear, with localised tenderness. Weakness in ankle ‘plantar flexion’ is also present.
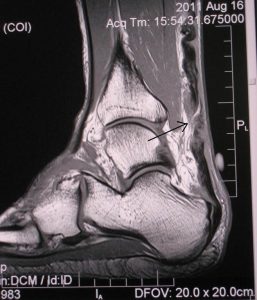
While the diagnosis is often made based on a clinical history and examination alone, often an ultrasound or MRI scan is performed to confirm the ‘level’ of the injury, and any associated degeneration within the tendon.
Achilles Tendon Rupture Treatment
What are your options?
All Achilles tendon ruptures should be managed actively. An early diagnosis and management plan is required for optimal outcome. There are two board groups of treatment options.
Nonoperative Treatment
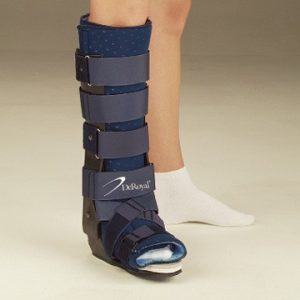
This involves the use of a CAM boot and protected weight bearing with crutches. The addition of ‘heel wedges’ are used to help approximate the tendon ends whilst healing occurs. The CAM boot is typically required for 10 weeks, with gradual removal of the ‘heel wedges’ over time.
Surgical Repair of the ruptured Tendon
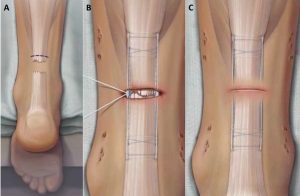
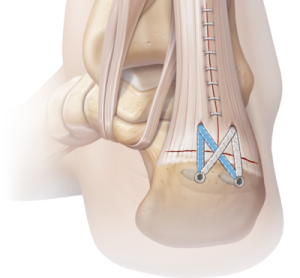
Surgical repair of the achilles tendon allows a direct ‘end to end’ repair of the torn tendon. This technique reduces the risk of sustaining a repeat rupture of the tendon, and maximises future ‘push-off’ strength of the calf muscles. Our Surgeons perform this via a minimally invasive technique.
Achilles Tendonitis | Tendinosis
What you need to Know
Achilles Tendinosis
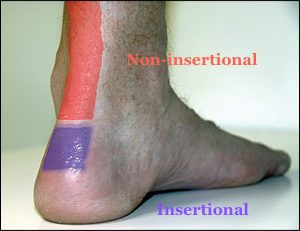
There are 2 types based on the exact location
Non-Insertional Achilles Tendinosis
This condition results in degeneration of the middle area (mid-substance) of the achilles tendon. This is typically seen in younger active people and can be very debilitating.
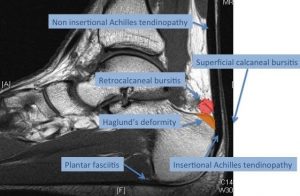
Insertional Achilles Tendinosis
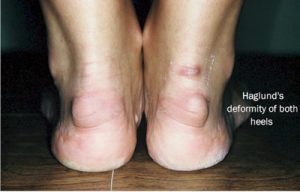
This condition relates to degeneration of the tendon as it inserts into the heel bone (calcaneus). It may be present in association with a bony bump (Haglund deformity) at the back of the heel and bursitis.
What are the symptoms
Patients typically present with chronic (long-term) pain at the back of the heel, which is often exacerbated by exercise. A feeling of ‘tightness’ of the calf muscles is usually present, and patients often notice a ‘bump’ or enlargement of the tendon. Difficulty with shoes rubbing is common.
What Imaging is needed
A plain xray assesses the degree of bony protuberance that is present, and any additional pathology such as arthitis is looked for. An MRI scan is the best imaging modality to assess the integrity of the achilles tendon itself. The location and severity of the degeneration is seen.
Achilles Tendinosis Treatment
Achilles tendinosis is best managed with an active management plan.
An initial period of ‘rest’, anti-inflammatories, and achilles stretching, is followed by a structured strengthening program.
If the symptoms fail to settle, surgical debridement of the degenerative tendon and removal of any excess bony protuberance or bursitis (inflamed tissue) is performed.
Do you experience any of the following?
Pain over your achilles tendon
Tightness of your calf muscles
A bony prominence at the back of your heel
Ankle sprains and arthritis
People don’t generally tend to associate ankle sprains with ankle arthritis due to its seemingly innocuous presentation in comparison to ankle fractures or dislocations, however recurrent ankle sprains can result in serious trauma to the ankle. Post traumatic...
A seemingly simple ankle sprain can lead to ankle arthritis
Ankle arthritis is less common that Hip and Knee arthritis. In fact, while Hip and Knee arthritis is commonly attributed to genetics and ‘wear and tear’ with increasing age, the ethology of ankle arthritis is often quite different. The most common cause for someone...
Ankle Impingement
Ankle impingement is a common cause of ankle pain. We discuss what causes ankle impingement here.
Disclaimer: Please note that this is general advice only - for more information, please consult your regular doctor, or obtain a referral to see a specialist orthopaedic surgeon.
Orthopaedics 360
Orthopaedics 360
P: (08) 7099 0188
F: (08) 7099 0171
Southern Specialist Centre
Orthopaedics 360
P: (08) 7099 0188
F: (08) 7099 0171
Health @ Hindmarsh
Orthopaedics 360
P: (08) 7099 0188
F: (08) 7099 0171